
Chronic prostatitis is an inflammatory disease characterized by lesions of the prostate gland and severe urodynamic disorders. One of the causes of chronic inflammation of the prostate is improper or untimely treatment in the acute stage, when the desquamation and proliferation of the glandular epithelium are reversible and are successfully corrected by drugs within 2-3 weeks.
Treatment of chronic prostatitis includes massive antibiotic therapy aimed at eradicating the infectious pathogen, a number of measures to increase the body's immune resistance, physiotherapeutic methods, thermotherapy. Psychocorrection can also be included in the treatment regimen, as neurasthenic and neurosis-like states are often observed in men with long-term and recurrent prostatitis.
Why does inflammation become chronic?
Knowing the causes of chronic inflammation of the prostate is necessary to prevent exacerbations and improve the quality of life of patients. There are a number of factors that can affect the functional state of the glandular (glandular) tissue of the prostate gland and cause inflammation, which is based on peeling and proliferation of epithelial cells.
The main cause of chronic prostatitis in men is the extensive contamination of the mucous membranes of the genitourinary system by pathogenic microorganisms. In the vast majority of cases (over 80%) of infectious prostatitis, gram-negative and gram-positive bacteria become the causative agent of infection: enterobacteria (in particular, Escherichia coli), gonococci, staphylococci. Less often, the infectious and inflammatory process proceeds against the background of infection with viruses, fungi and protozoa, but such forms of prostatitis are successfully treated during the acute period and rarely give relapses, subject to correct and timely therapy.
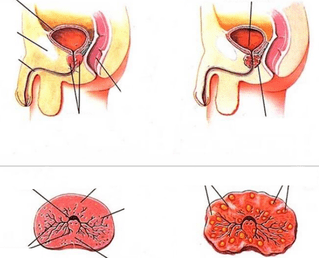
It should also be borne in mind that a single acute urinary tract infection is sufficient for the development of chronic aseptic prostatitis, therefore, personal hygiene, use of condoms during intercourse and timely treatment of diseases of the tracturinary tract are of great importance in the prevention of this disease in men. Medicine knows cases of hematogenous (through systemic circulation) infection of the prostate in chronic sinusitis, tonsillitis and other diseases that contribute to the active growth of pathogenic flora, therefore, the hygiene of foci of chronic infection is an important stage in the complex treatment forprolonged or protracted inflammation of the prostate.
Negative factors that can cause exacerbation of prostatitis (including non-infectious course) are:
- lesions of the urinary tract and surgical interventions on the organs of the genitourinary system;
- Regular or severe hypothermia of the pelvic organs (swimming in open water in periods when the water is not hot enough or the weather is cool outside, working in refrigerators and freezers, etc. );
- hypodynamia caused by sedentary work and insufficient physical activity of a man (a sedentary lifestyle is one of the main factors in the development of chronic cognitive prostatitis);
- bad habits, in which the absorption of the most important macro and microelements that determine the chemical composition and rheological properties of the prostate secretion (zinc, chromium, selenium, manganese) is slowed down or compromised;
- disturbances in the intimate sphere (frequent masturbation, irregular sexual intercourse, long periods of abstinence, frequent arousal that does not end with intercourse);
- overweight;
- eating disorder (increased consumption of spicy, too salty, smoked and fatty foods).
Be careful! Urologists note that the main pathogenetic factor in the development of chronic inflammation of the prostate gland is posterior urethritis. It has also been noted that inflammatory changes in the prostate in men appear during the first few months after suffering from a gonorrhea infection.
Treatment of chronic prostatitis with drugs
Treatment of chronic prostatitis with drugs is aimed only at suppressing acute symptoms during an exacerbation and destroying the infection, but drugs cannot be used as the only means (the effectiveness of such treatment will not exceed 36%, according to Dr. Pechersky).
A comprehensive drug treatment regimen for protracted or recurrent prostatic inflammation, which is used today as a standard in uncomplicated diseases, is presented in the table below.
Table. Preparations for the complex treatment of chronic prostatitis.
| Pharmacological group | Purpose |
|---|---|
| Antibiotics of the macrolide group, semi-synthetic penicillins and third generation cephalosporins with a broad spectrum of antibacterial activity. | Eradication (destruction) of pathogenic bacteria - causative agents of infectious prostatitis, urethritis, cystitis and other urinary infections. |
| Antimicrobial and antiprotozoal agents. | Treatment of infections caused by pathogenic microbes and protozoa. |
| Non-steroidal anti-inflammatory drugs (preferably in the form of rectal suppositories). | Reduction of inflammation in the tissues of the prostate, relief of pain in the perineum, intergluteal space, sacrum and groin. |
| Antiseptics in the form of rectal suppositories. | Rehabilitation of the rectal mucosa and prevention of its infection with prolonged prostatitis. |
| Alpha blockers. | Normalization of urination, restoration of daily urine output. |
| Correctors of the microcirculation. | Elimination of congestion in the vessels of the small pelvis, restoration of normal blood and lymphatic flow. |
| Correctors of urodynamics (agents that affect metabolism in the tissues of the prostate). | Improvement of metabolic and metabolic processes in the tissues of the prostate gland and its nutrition. |
| Power regulators. | Complex treatment of erectile dysfunction, improvement of chemical composition, viscosity and fluidity of seminal fluid, increase in spermatic activity (the use of drugs of this group is indicated for patients whose prostatitis is complicated by autoimmune infertility). |

The duration of antibiotic treatment is at least 4-6 weeks. In no case should you take antibacterial drugs without a prescription, since the main factor in the selection of therapy is the results of microscopic examination of the secretion of the prostate and spontaneously released fluids as a result of prostate massage. Some antibiotics, for example, penicillins (a combination of amoxicillin with clavulanic acid) are reserve drugs, and their incorrect use can lead not only to the absence of a clinically significant effect and the progression of the pathology, but also to the development of superinfection.
Important! In some cases, men with chronic prostatitis need psychocorrection, especially if the pain syndrome is combined with behavioral changes, increased anxiety, irritability, and neurasthenia. To suppress these symptoms, antidepressants with selective inhibition of serotonin reuptake are used.
Physiotherapy
Heat therapy is the main method for the treatment of chronic prostatitis outside the periods of exacerbation (after the regression of acute symptoms). Heat therapy refers to physiotherapy methods and is a dosed effect of heat on the affected area. The benefits of thermal procedures are in the normalization of blood circulation, relief of inflammatory processes, reduction of chronic pelvic pain, which is one of the main clinical manifestations of chronic prostatitis, which reduces the quality of life of men. Heat also improves the penetration of medicinal substances into the prostate tissue, therefore, in some cases, physiotherapy is used to increase the effectiveness of drug therapy (for example, electrophoresis with antibiotics). For men at high risk of thrombosis, rewarming is prescribed for prevention, since heat has a moderate resorption effect.
There are a number of methods of thermal effects on the body, and the choice of a specific treatment method should be carried out by a doctor, taking into account the clinical picture, form and stage of the disease, the age of the man and hisindividual tolerance. The most effective methods of heat therapy for prostatitis are:
- thermal applications with minerals (ozokerite, paraffin, bischofite), salt or sand;
- electric heating plates;
- deep heating of highly resistant tissues for a direct action on blood vessels and nerve endings (diathermy);
- exposure to high-frequency alternating magnetic fields to eliminate pain, relieve inflammation and eliminate neurosis-like manifestations (inductothermy);
- ultrasound therapy (promotes resorption of abscesses and healing of formed scars);
- electrophoresis with the introduction of electrodes into the rectum;
- impact on prostate tissue with high frequency impulse currents (darsonvaluation).
In some physiotherapy rooms, chronic inflammation of the prostate is treated with hot mud applications ("mud pants"). Such procedures have a positive effect not only on blood and lymph circulation, but also on the production of prostatic secretion, as well as on the nutrition of the tissues of the inflamed organ. In some cases, mud is injected directly into the rectum in the form of tampons, since with this method of administration it is possible to quickly achieve a therapeutic effect and a positive response to therapy.
Other treatments
The complex treatment scheme, in addition to drug and heat therapy, is supplemented by various procedures that the doctor prescribes, taking into account the peculiarities of the pathology in each case.
Prostate massage
This is one of the main methods of treating chronic inflammation of the prostate gland, which is advisable to use in almost 90% of cases (in the absence of contraindications). Massage is an effect of the finger on the prostate to stimulate the outflow of secretory fluid. The duration of the procedure is usually about 1-2 minutes. The criterion for a sufficient effect is the complete emptying of the prostate glands, which the patient feels as a relief (about which he should inform the doctor).
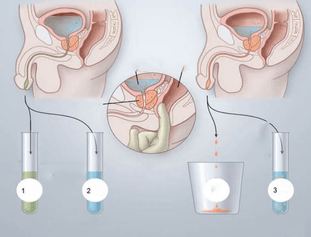
The benefits of the massage are determined by the therapeutic effect that can be obtained after undergoing a course of treatment (8-12 procedures). With a simple course, these are:
- normalization of muscle tone;
- improvement of blood circulation in the prostate vessels (due to this, the transport of medicinal substances into the tissues of the affected organ is accelerated and the effectiveness of therapy increases);
- restoration of secretory patency;
- normalization of the outflow of blood and lymph from the prostate gland (especially significant in cognitive prostatitis).
The procedure is contraindicated during the acute period due to the high risk of spread of infection to surrounding tissues and organs (hematogenous infection), with other infectious diseases of the genitourinary system, the presence of cysts or stones in theprostate. Prostate massage is not prescribed for patients who have been diagnosed with tuberculous organ damage, adenoma, or other neoplastic diseases (including cancerous lesions of the prostate gland). In the presence of rectal diseases (hemorrhoids, anal fissure, proctitis, paraproctitis) massage can cause complications and cause a relapse of the underlying disease.
Important! Studies show that nearly 42% of men refuse prostate massage due to the increased psychological distress associated with the peculiarities of this procedure. The physician's work with such patients should include detailed information on the consequences of refusing treatment and on possible complications, especially infertility and persistent sexual dysfunction. In some cases, it may be advisable to prescribe mild sedatives a few days before starting treatment.
Warm enemas
Warm enemas are home treatments for chronic prostatitis, but urologists recognize their effectiveness and recommend them for faster and more effective treatment of prostatitis. The water temperature for these enemas should be around 42 ° C. Before the procedure, it is necessary to cleanse the intestines with a regular enema or laxatives. The volume of an enema is from 150 to 300 ml. It is recommended to empty the intestine 30-50 minutes after administration of the solution.

Recipes for chronic prostate inflammation are listed below.
- Dissolve 10 drops of iodine and approximately 20 ml of chlorhexidine in 200 ml of water. Apply at bedtime for 15 days.
- A decoction of chamomile, St. John's wort or calendula (about 250 ml) should be introduced into the rectum and kept for 1 hour. The procedure is repeated once a day for 2 weeks.
- Sea buckthorn oil (40-50 ml) is heated to 40 ° C and introduced into the rectum for 20-30 minutes. The course of treatment is 10-15 days. The procedure is best done before bedtime.
- In case of severe pain syndrome, which significantly limits the patient's mobility and worsens his quality of life, microclysters with novocaine can be used. Dissolve 2 ampoules of 2% novocaine solution in 180 ml of a steep decoction of chamomile. Hold the position for at least 50 minutes. Repeat every day for 1 week.
Anti-inflammatory drugs, antiseptics, antibiotics can also be used by medicines for microclictors. The use of these drugs is allowed with the permission of a doctor strictly in the indicated dosage.
Treatment of chronic prostatitis: step by step instructions
The use of various methods of treatment is not enough to completely get rid of chronic prostatitis. If a man does not control his diet and change his lifestyle, exacerbations will occur regularly, leading to irreversible changes in the structure and functional activity of the prostate glands and persistent dysuric and sexual disorders. In order for the effectiveness of treatment and the duration of remission to be greater, the recommendations set out in the following instructions for patients with chronic prostatitis should be followed.

- Step 1. If a man is diagnosed with chronic prostatitis, he should start by correcting his diet. It is necessary to exclude from the menu foods with a large amount of fat, salt and spices. Fats increase blood cholesterol levels and salt promotes fluid retention and edema in the prostate tissue. Spices (like various chemical additives) irritate the mucous membranes of the urinary tract, causing an exacerbation of existing symptoms.
- Step 2. It is also necessary to completely eliminate alcoholic beverages, as they slow down the absorption of nutrients, disrupt the circulation of blood and lymph and negatively affect the metabolism in the prostate. If a man suffers from tobacco addiction, it is necessary to take measures to get rid of this habit (toxic substances in tobacco smoke violate the viscosity and fluidity of prostatic secretions and change their chemical composition).
- Step 3. Overweight men should consult an endocrinologist and nutritionist for a complete diagnosis and correction of body weight, taking into account the identified deviations. Obesity is the most important factor in the development of chronic prostatitis and an important stage in complex therapy is weight loss in patients with high BMI.
- Step 4. To eliminate congestion associated with hypodynamic disorder, an adequate level of physical activity, corresponding to age and fitness, must be provided. Swimming, physiotherapy exercises, stretching exercises, walking are useful for prostatitis.
- Step 5. For normal functioning of the prostate, it is necessary to monitor the quality of sexual life. It is advisable to have a permanent sexual partner, to avoid episodes of sexual arousal if there is no possibility of further intercourse and to be regularly checked for genital infections, which can also lead to an exacerbation of chronic prostatitis.
Men with recurrent prostatitis need to monitor emotional distress, avoid stressful situations, as well as prolonged exposure to cold or drafts.
Chronic prostatitis is a difficult disease to treat, especially if the patient does not follow the doctor's prescription and does not take a responsible approach to diet and diet problems. Inflammation of the prostate is dangerous with serious complications, so it is necessary to approach the problem comprehensively. Men with this diagnosis should understand that pills alone are not enough to fully restore all functions of the prostate gland, so you should not abandon the basic therapy methods for chronic prostatitis suggested by your doctor, even if they cause psychological distress orprimary physicist.
































